[ad_1]
A large group of researchers has reviewed the literature related to acute flaccid myelitis (AFM) and has summarized current knowledge of this illness in a new consensus document.
In it, researchers describe the epidemiology and potential causes of AFM, the disease’s clinical presentation, the methods required to diagnose it, effective strategies for acute management, and considerations for long-term rehabilitation.

Dr Carlos Pardo
The authors intended “to achieve a consensus for diagnosis and management of AFM to facilitate better and more effective care of patients affected by this disorder,” Carlos A. Pardo, MD, professor of neurology and pathology at Johns Hopkins University School of Medicine, Baltimore, Maryland, told Medscape Medical News. “The final goal is that any healthcare provider around the world be aware about AFM, the diagnostic criteria, and acute management and care of the long-term consequences of AFM.”
The incidence of AFM has increased since 2012, and the disease should be regarded as a major global public health concern, the authors write. The possibility of future AFM outbreaks makes it necessary to increase awareness of the disease and educate clinicians about diagnosis and treatment, they note.
Questions that remain unanswered include how common exposures such as enterovirus infections cause severe neurologic disease, what the optimal therapeutic approach is, and whether prevention is necessary.
The review was published online January 23 in The Lancet.
Table of Contents
Pleocytosis Common
AFM is a disabling disease that resembles polio and mainly affects children. It has been diagnosed around the world and often occurs in geographical clusters. Researchers suspect that the D68 enterovirus causes the seasonal, biennial outbreaks that have been observed.
Other enteroviruses, such as A71 and coxsackievirus strains, also may cause AFM. Defining the disease by its associated organism may not be appropriate for clinical practice, however, inasmuch as D68 may be detectable only at an early stage of the disease, the authors write.
The median age of patients with AFM is 6.3 years. Most experience a prodrome marked by fever and respiratory symptoms, such as cough, rhinorrhea, or pharyngitis, they note. Neurologic symptoms generally begin 1 to 10 days after the onset of the prodrome.
Patients develop flaccid weakness and hyporeflexia or areflexia in one or more limbs. Onset typically is asymmetric and favors the upper limbs and proximal muscles. Patients also may have weakness of the neck, trunk, diaphragm, or other respiratory muscles. Most patients require hospitalization, and some need intubation.
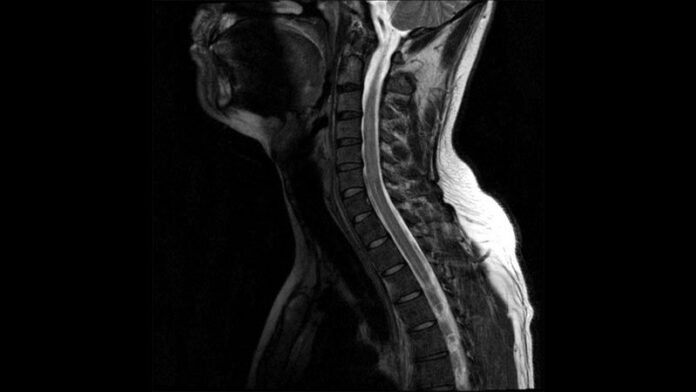
The most useful diagnostic test, the researchers suggest, is MRI of the spinal cord. The characteristic finding in AFM is T2 hyperintensity of the spinal cord gray matter. Spinal cord gray matter lesions tend to be longitudinally extensive. The cervical cord is the most commonly affected.
For almost all patients, lumbar puncture reveals cerebrospinal fluid (CSF) pleocytosis, the authors note. The white blood cell count is mildly to moderately elevated; levels resolve over several weeks. In the acute phase, CSF analysis helps distinguish AFM from other causes of flaccid paralysis that are less likely to cause pleocytosis.
Identifying the causes of AFM or its mimics requires investigation outside the central nervous system or CSF, they note. Respiratory samples may indicate enterovirus D68, and stool samples may indicate enterovirus A71. Electromyography or nerve conduction studies often are not required for diagnosis.
Early management of AFM centers on supportive treatment. This includes securing the airway, treating autonomic dysfunction, managing pain, preventing the complications of acute immobility, and beginning early rehabilitation. The pathophysiology of AFM is incompletely understood, and no medical therapies have been studied in prospective, controlled trials. Intravenous immunoglobulin often is administered because the primary cause of AFM is believed to be viral infection.
Residual Impairment
After remission, many patients with AFM develop residual impairment. Data suggest that fewer than 10% of patients achieve full recovery. Electromyography, nerve conduction studies, and MRI could help predict patients’ outcomes.
Recovery in the limbs appears to progress from distal to proximal areas. The worst-affected muscle groups are the least likely to recover. Deaths from AFM are rare. Although rehabilitation can lead to continuing functional recovery, patients may have neurologic, musculoskeletal, or psychological sequelae.
“Prognosis and outcome biomarkers of AFM are not very well established,” said Pardo. “However, the magnitude of MRI abnormalities within the spinal cord during the acute stage and the need for critical care management and mechanical ventilation are perhaps the most recognized factors that identify poor outcomes.”
The most urgent focus of research is the mechanism of AFM pathogenesis, said Pardo. Investigators also are searching for reliable tools for the rapid laboratory diagnosis of AFM. These tools may identify viruses or diagnostic biomarkers. Another priority of research is the identification and development of treatment approaches for limiting the rapid progression of neurologic damage after symptom onset, said Pardo.
Comprehensive Review
“This is the most comprehensive review [of AFM] published to date,” Marc C. Patterson, MD, professor of neurology, pediatrics, and medical genetics at Mayo Clinic Children’s Center, Rochester, Minnesota, told Medscape Medical News. “The review emphasizes the importance of considering this diagnosis in any child with weakness, particularly asymmetric weakness, and provides useful guidance in differentiating alternative diagnoses.”

Dr Marc Patterson
Recognition of AFM has improved significantly in recent years, although it remains a challenge, Patterson added. “Access to the appropriate diagnostic tests represents a continued unmet need, particularly in resource-poor areas,” he said.
A majority of patients who are exposed to the virus may be mildly affected, and the biggest unanswered question may be which host factors predispose a patient to develop severe disease.
“These are not new questions; in the age of polio pandemics, only a minority of susceptible individuals developed severe neurologic disease,” said Patterson. “If we understood the host factors (presumably related to genetically determined variations in individual immune systems), it might be possible to recognize highly susceptible individuals and to tailor specific therapies for them.”
The review was supported by the Siegel Rare Neuroimmune Association and the Bart McLean Fund for Neuroimmunology Research. Pardo is an unpaid advisor to the AFM Task Force of the Centers for Disease Control and Prevention. He receives support from the National Institutes of Health and the Bart McLean Fund for Neuroimmunology Research. Patterson has disclosed no relevant financial relationships.
Lancet. Published online January 23, 2021. Abstract
For more Medscape Neurology news, join us on Facebook and Twitter.
[ad_2]
Source link