[ad_1]
Editor’s note: Find the latest COVID-19 news and guidance in Medscape’s Coronavirus Resource Center.
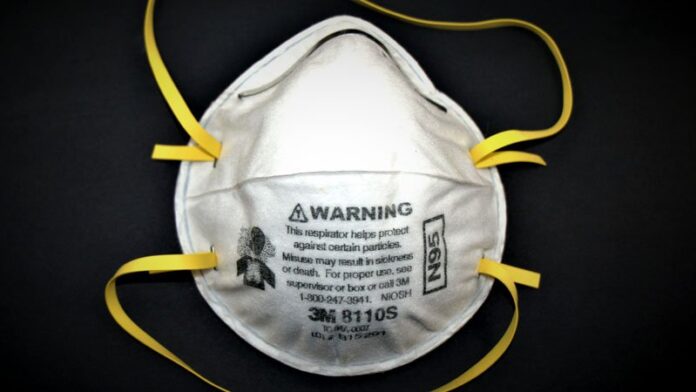
Abraar Karan, MD, has been treating COVID-19 patients for 10 months. In that time, he hasn’t gotten the virus, and he credits his N95 mask for protecting him.
“I’ve seen more COVID patients than I can count since March, and I get tested regularly, and I’ve not tested positive. I want others to have that kind of protection, too,” says Karan, an internal medicine doctor at Brigham and Women’s Hospital and Harvard Medical School.
But N95 masks are in short supply, and Karan says he’s frustrated that high-filtration, or hi-fi, masks aren’t available for the public nearly 1 year into the coronavirus pandemic. Karan recently co-authored an op-ed highlighting his concerns and calling for a national initiative to make masks with higher filtration easier to get — even having the government send them to people’s homes.
With a mask that has good enough filtration for personal protection & source control— you are functionally a dead end for the virus.
Either you no longer transmit it onwards or you never get infected, ideally the latter. And regardless of variants, Hi-Fi masks protect you.
— Abraar Karan (@AbraarKaran) January 16, 2021
The issue is as relevant today as it was a year ago when the first cases of the coronavirus were identified in the United States. A study released Tuesday in The Lancet found that a 10% increase in mask-wearing makes it 3 times as likely that the coronavirus spread slows.
He says the US needs a more coordinated effort to do two things: protect those wearing masks from getting the virus, and prevent those who have the virus from emitting the droplets and aerosols that spread COVID-19, especially when they’re asymptomatic and don’t know they’re infected.
“We’ve been saying wear a mask, wear a mask. Well, we’re now 10 months into this, and we are still just telling people to wear masks that are OK, but they’re not the best protection that we can get. We already know that N95-level protection is out there and it is the best,” Karan says. “There is a supply issue — so fix it.”
Karan says many other countries are taking steps to get better masks to their citizens. In Austria, the government says it will distribute free FFP2 masks (their equivalent of N95s) this month to people over the age of 65. Karan isn’t the only one with this idea. Researchers recently raised the question in The Atlantic, too — pointing out that cloth masks were supposed to be a “stopgap measure” in the US and that other countries have done far more to get better masks into the hands of their people. Examples include Hong Kong giving lab-tested six-layer masks to the public, Taiwan boosting its mask production to get more high-quality masks to people on a weekly basis, and Germany now requiring people to wear higher-grade masks.
“We are 10 months into this. We should have more comfortable designs that have a higher filtration efficacy,” Karan says. “I’ve talked to some companies that are working on different mask designs now, trying to get more filters into cloth masks that can provide some electrostatic charge that can stop small particles.”
Engineering problems need to be overcome, but at this point, Karan says, “it’s frustrating that we still don’t have products that are going out at any level of scale. How many times have you heard leaders saying, ‘Wear a mask,’ ‘Wear a mask’? It’s easy to say wear masks. Why are we not talking about better masks?”
Table of Contents
Are Fabric Masks Enough?
The CDC recommends that people wear masks in any public setting — including on buses, trains, and airplanes; at events; and when they’re around others. Multiple studies show that COVID transmission goes down when people wear masks — 45% in 20 days in one study in Germany. The CDC has also shared data from Arizona and Kansas showing COVID transmission rates falling in areas where mask mandates are put in place.
The CDC doesn’t recommend N95s for the public but does suggest masks that:
-
Have two or more layers of washable fabric
-
Completely cover your nose and mouth
-
Fit snugly against your face without gaping
But more and more, other health experts are saying this guidance isn’t enough and more protection is needed.
“Last year, it was important to get as many people to wear masks as possible; something was better than nothing. Now, it’s time to improve our masks because of B.1.1.7, etc.” tweeted Linsey Marr, PhD, an engineering professor at Virginia Tech who specializes in airborne transmission of viruses. In another tweet, she explained the need for multiple levels of protection against the virus, writing, “Yes, vaccines are here, but so is B.1.1.7. We need to up our mask game…. N95s for all.”
Here's a great article by @zeynep and @jeremyphoward about improving our masks. Last year, it was important to get as many people to wear masks as possible; something was better than nothing. Now, it's time to improve our masks because of B.1.1.7, etc.https://t.co/Fv8UjBCTuA
— Linsey Marr (@linseymarr) January 13, 2021
“B 1.1.7” is a so-called “super strain” of the coronavirus first identified in the United Kingdom. Estimated to be 70% more contagious than the previous coronavirus strain, the variant is sprinting across the United States.
Former CDC Director Tom Frieden, MD, is another public health expert raising concerns. The infectious disease doctor tweeted on the subject a few times in 2021, stressing the need to boost public protection. On January 10 he posted: “Almost any mask greatly reduces spread from someone with the virus. But to protect ourselves better, we may need N95/KN95 when indoors near others. A more infectious strain requires stronger defenses.”
4. Mask up. Almost any mask greatly reduces spread from someone with the virus. But to protect ourselves better, we may need N95/KN95 when indoors near others. A more infectious strain requires stronger defenses. Masks all the time when around others not from your household. 15/
— Dr. Tom Frieden (@DrTomFrieden) January 10, 2021
“It’s possible that as more is learned about more transmissible variants, mask quality will be even more important,” Frieden told WebMD.
Not all situations are the same, Karan says. “There are certain situations where COVID is more efficiently transmitted by small particles that float in the air and remain in the air. And those situations are poorly ventilated, crowded indoor situations that we increasingly find ourselves in — mass transit, grocery stores, pharmacies, shops, elevators,” he says. “Telling people to wear masks that are just OK isn’t providing the best protection in these locations. We should be offering more.”
Karan acknowledges there are many challenges with N95s. While they offer the most protection, not only are they in short supply and largely reserved for healthcare workers right now, but many doctors also say they’re not especially practical for the public. Healthcare workers get specially fit for them. They’re not comfortable for long periods of time, and they’re expensive, too.
“They shouldn’t be the only option out there,” Karan says. “We should be having public-private sector partnerships that are pushing for masks that are beyond what we’ve had before. There needs to be some innovation in this space, because if you get the right protection on people, that can stop transmission and substantially reduce the number of potential people that get infected.”
So What Kind of Mask Should You Wear Now?
If you’re looking to protect yourself from COVID, what is the best mask for this moment? Frieden ranked them for WebMD.
“N95 masks are the most protective masks, followed by three-ply surgical mask, then a fabric mask. A fabric mask is a lot better than no mask. In certain situations, such as an immunocompromised person in an indoors health setting, an N95 mask, properly fitted and worn, is optimal because it provides the most protection. Fabric masks offer less protection than other masks. Some protection is better than no protection.”
Marr and Monica Gandhi, MD, an infectious disease doctor and professor of medicine at the University of California, San Francisco, compared 10 masks and wrote about their findings in the journal Cell. Based on their research, they say fabric masks of at least two layers provide basic protection. For maximum protection, they recommend wearing two masks — layering a cloth mask (for an extra layer of filtration and increased fit to the face) and a surgical mask, which also acts as a filter, too.
“I think that we’re at a point where I would nuance the message of wearing a mask to say here is a mask option for maximal protection that will likely block more and come close to simulating N95s. My heartiest recommendation is for a surgical mask and a cloth mask together,” Gandhi says. “I would not say there’s a hard-and-fast rule about this, and I’m not advising young people to necessarily do this. But it does give an option for people who can’t get an N95, have some sort of vulnerability, live in areas with high transmission rates, have to work indoors around others, or have a great level of concern about this virus.”
Gandhi says scientifically, it doesn’t matter which mask you put on first. She suggests basing that decision on comfort or which one you’re trying to make last longer. She recommends having the cloth mask against your skin and the surgical mask on top. “You can wash the cloth mask more readily, and the surgical mask you could use literally for a full 7 days, probably before it loses its give,” she says.
Gandhi says she is most concerned about the many mask options out there and how confusing it can be for people trying to figure out what provides the most protection. “I’m a clinician at heart, and I think we just have to try to make it more simple for people,” she says.
Alice Sato, MD, an assistant professor of pediatric infectious diseases at the University of Nebraska Medical Center in Omaha, agrees. She is having a lot of discussions about face masks these days with young patients and their families and says until better options are easier to get, she just stresses to her patients that the best mask right now is one you’re actually willing to wear.
“Any type of effort to wear a mask works better than none,” she says. “We should encourage people to wear the best face covering they have, as much as they can, particularly indoors. If we as a country can help provide better masks, though, we should.”
Sato, who’s also an epidemiologist at Children’s Hospital & Medical Center in Omaha, tells patients that the fit of the mask makes an enormous difference, too. “We need people to wear the mask appropriately, and that means it conforms to your face at your nose, under your chin, and on your cheeks rather than gaping and letting air in,” she explains. “Double layering is adding extra filtration, but a lot of the benefit also comes in making sure you are covering those gaps around the mask, because not every mask you put on fits equally.”
Karan says he understands there has to be wiggle room for the real-world moment, but he stresses just how frustrating it is to ask people to figure out how to improve protection on their own this far into a global pandemic.
“Everyone can maneuver and ‘MacGyver’ a mask at home, but I can’t sit here and say that mask is going to be good. There is some serious engineering that goes into these. You can’t just take a few pieces of cloth and put it together and have the fit and filtration of an N95,” he says. “After 10 months, there really should be some level of federal coordination so that people can easily get the kind of masks that best protect them.”
[ad_2]
Source link